A tooth extraction does not stop once the tooth is out. From that very moment, the jaw begins to change, quietly and often without obvious symptoms.
Bone remodeling is a natural response that happens to everyone to some degree. The problem is when that loss goes unmanaged. Gradually, it can make future implants more complex and impact how your bite feels. It can even change facial balance. This is why we focus on education and timing. Understanding jawbone resorption following an extraction empowers you to act early, when preservation is most straightforward and predictable.
In this guide, we break down the natural changes step by step, explaining when smart intervention can secure your long-term options before they begin to narrow.
Why Bone Changes After a Tooth Is Removed
When a tooth is removed, the jaw loses more than meets the eye. The periodontal ligament, which once attached the tooth to the bone, is missing too, and that stimulation, day in and day out, is what keeps bone healthy. Without it, the body will naturally begin to remodel the area.
The outer, or buccal, plate is the most vulnerable because it is thin, and its blood supply changes rapidly after extraction. Bone loss is also related to location. The front teeth tend to resorb faster than the back teeth. The upper jaw acts differently from the lower. What the patients notice usually is minimal, while beneath the gums, the alveolar ridge resorption timeline has already begun.
The Natural Timeline: What Happens and When
After an extraction, the jaw follows a rather predictable pattern of healing. The first two weeks are spent recovering, during which a clot forms, early bone remodeling begins, and the gums start to close.
From weeks two to eight, bone loss is greatest, particularly in width, as the buccal plate resorbs more quickly. Between three and six months, the ridge continues to shrink in both height and width while the tissue stabilizes. After six months, changes are slow but continuous, and sinus expansion becomes a challenge in the upper jaw. This alveolar ridge resorption timeline explains why timing matters more than most patients realize.
How Much Bone Is Typically Lost (And Why It Matters)
Bone loss after tooth removal often follows a predictable pattern. The most significant extent of alteration typically happens during the first period; the horizontal width of the ridge disappears first, while the decline in vertical height generally follows thereafter.
Functionally, these alterations may affect denture stability, cause minor changes in occlusal function, or increase the tendency for food impaction. Aesthetically, reduced osseous volume compromises lip support, alters the smile line, and tends to darken interdental spaces. Procedurally, reduced bone often limits implant selection, demands additional grafting, and prolongs overall treatment time. Thus, understanding jawbone resorption after tooth loss is relevant to protecting both form and function.
Intervention Window #1: The Day of Extraction (Best Case)
The day a tooth is removed is often the best opportunity to protect what’s next. Socket preservation involves placing graft material into the site and covering it with a membrane to retain bone volume as healing commences. Sometimes, an implant can even be placed on the same day if the area is deemed stable and any infection is controlled.
Early intervention at this stage helps preserve natural contours, improves the ease of future restorations, and may reduce the need for additional surgeries. This early approach is particularly helpful in the smile zone for patients planning implants and for those with thinner bone, who are more susceptible to jawbone resorption after extraction.
Intervention Window #2: Early Post-Extraction (0–8 Weeks)
If a tooth has already been removed without grafting, the early healing phase gives you a meaningful chance to step in. Within the first few weeks, ridge preservation or minor bone augmentation can often support the area before major collapse sets in. Opting to act now usually means smaller grafts, faster healing, and better-quality tissue than waiting longer. It also keeps future implant planning more straightforward. Early intervention along this alveolar ridge resorption timeline can avoid complex reconstruction later. This window is all about timing and making decisions while options are still simpler and more predictable.
Intervention Window #3: Delayed Management (3–12+ Months)
Once bone loss has progressed for several months, treatment enters a phase of rebuilding. The lost structure now needs to be regained through techniques such as guided bone regeneration, ridge splitting, or the sinus lift for the upper back teeth. While these solutions are still quite effective, they generally involve more stages. Healing takes longer, the process is more involved, and costs can increase. It’s all about planning carefully and being upfront about the timeline. With staged treatment and clear expectations, we can build a strong foundation that lasts.
Factors That Accelerate Bone Resorption
Precipitating factors can contribute to post-extraction bone loss. Smoking and nicotine decrease blood supply and prolong recovery, whereas infected or traumatic extractions further stress the bone.
Naturally thin buccal bone, previous periodontal disease, and systemic conditions, including osteoporosis, some medications, and uncontrolled diabetes, are other risk factors. These risk factors enhance jawbone resorption following extraction and create a very compelling reason to be proactive with care. It is important that we comprehend these risks so that early intervention, wise treatment planning, and consideration of beauty and function can be initiated.
Diagnosis: How We Measure and Plan Precisely
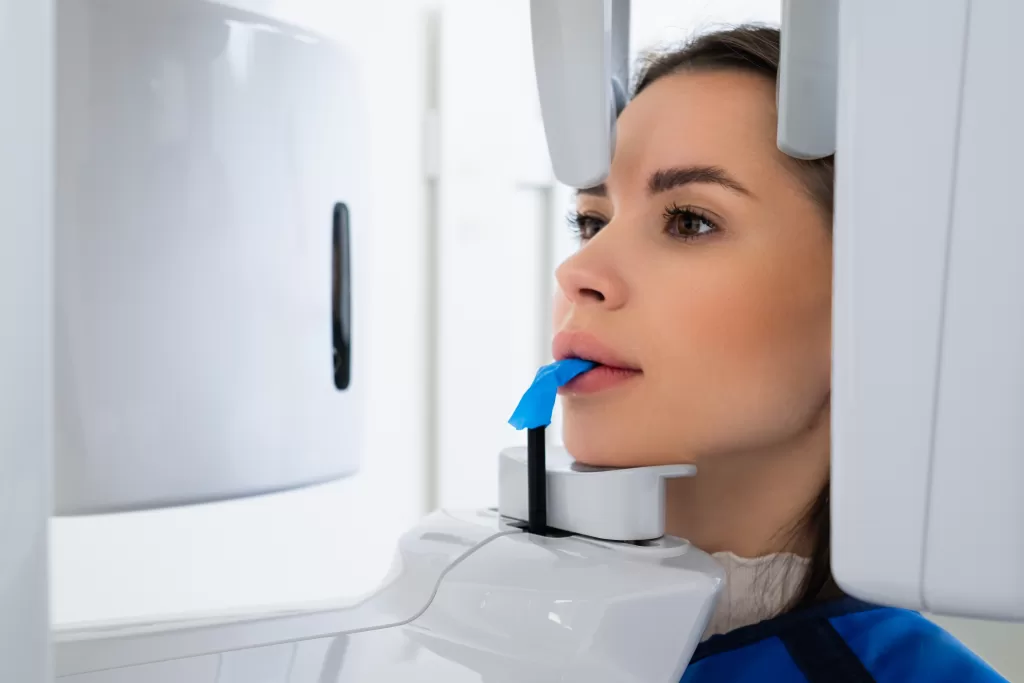
Getting the diagnosis right makes everything else easier. We, at the Ridge Oral Surgery clinic in New Jersey, start with a careful clinical examination, observing the ridge contour, tissue quality, and the area’s stability.
Imaging then fills in the details. Periapical X-rays provide a focused view, while CBCT scans allow us to measure bone width and height and map nearby structures with precision. We also plan around the final goal, whether that is an implant, a bridge, or a removable solution. Digital planning helps us anticipate changes in jawbone resorption after extraction, reduce guesswork, and design a treatment plan with fewer surprises and better long-term results.
What Patients Can Do Right Now
If you know an extraction is forthcoming, one of the best things you can do is inquire about socket preservation immediately. Planning on day one makes all the difference. If the tooth has already been taken out, book an evaluation a few weeks rather than months down the line. That early check helps us understand where you are in the timeline of alveolar ridge resorption.
At home, keep the area clean with gentle hygiene, avoid smoking, and closely follow postoperative instructions. Nutrition also plays a role in healing. Eat a protein-rich diet with enough vitamin D and calcium to support bone and tissue healing. Small, preventative steps now can save options later.
Our Approach to Preserving Your Jaw
Bone changes begin sooner than most people realize, often right after a tooth is removed. The best outcomes usually come from understanding what is happening early and acting before problems show up. Paying attention to the timing of alveolar ridge resorption preserves treatment options and simplifies future procedures.
At Ridge Oral Surgery, we help guide our patients through these decisions with clarity and sensitivity. If you are planning an extraction or have recently had one, scheduling a consultation now can help identify the ideal window to intervene and protect your long-term results.