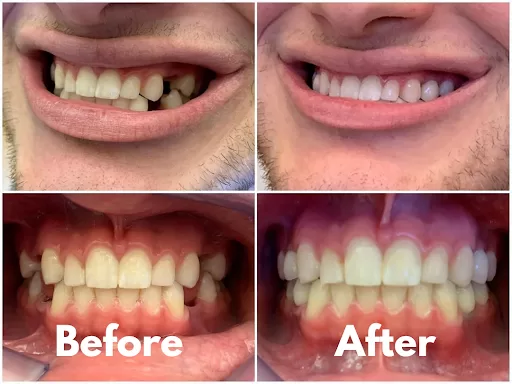
A healed fracture should not stop you from achieving a full smile. It means that timing and good planning matter a little more.
In case of jaw trauma, quite logically, one of the first questions that might arise is whether dental implants are still an option. Fortunately, many patients are candidates for implants after a jaw fracture once stability and bone quality are confirmed. With proper evaluation, stabilization, and thoughtful treatment planning, implants post-trauma often become a very viable option.
In this guide, we’ll walk you through candidacy, the imaging you may need, grafting possibilities, expected timelines, potential risks, and what recovery usually looks like, so you feel informed and confident about your next steps.
Are You a Candidate? The Trauma-to-Implant Checklist
We use a simple checklist to determine whether someone is a good candidate for dental implants after an injury. First, the fracture must be fully healed, and your bite should feel stable. That gives us a strong foundation from which to work. We need to verify that you have sufficient bone and healthy soft tissue; both are essential for long-term success.
We ensure there is no active infection and are frank about discussing issues such as tobacco use or medical conditions that might impede your recovery. We then align all of this with your goals. You may need to replace only one tooth or restore a larger area. Either way, this helps us in planning the right approach for you.
Imaging and Diagnostics That De-Risk the Plan
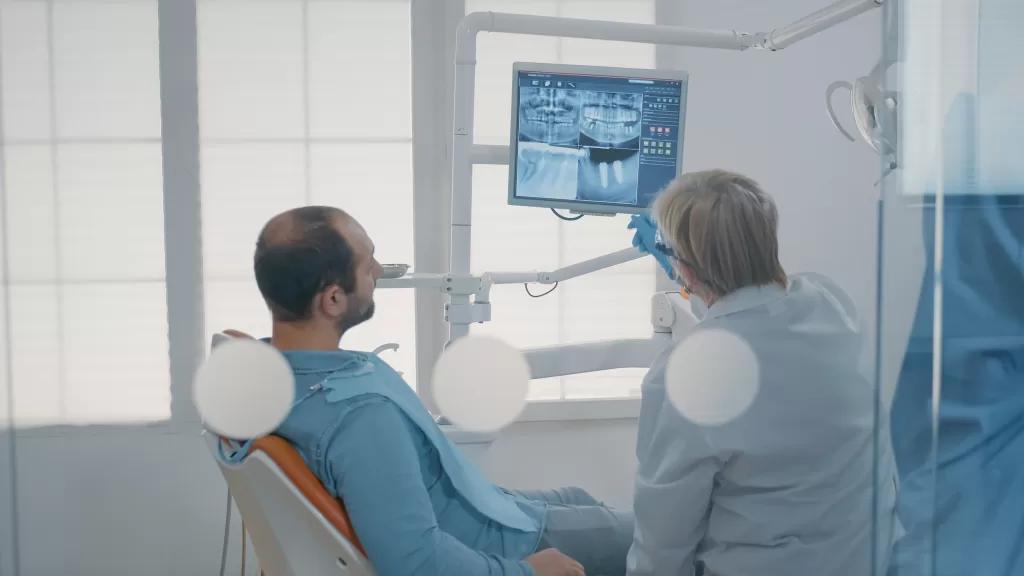
Once we feel you will be a good candidate, we move into the diagnostic stage to learn what your jaw looks like on the inside.
A CBCT scan provides us with that clarity. It helps us see any leftover defects from the fracture, the position of important nerves, how close we are to the sinuses, and whether any hardware from your treatment is still in place.
We also pay close attention to bone density and quality around the old fracture site and in areas where an implant may be placed. This gives us an idea of the area’s strength and supportiveness. From there, virtual surgical planning helps us map the ideal angle and length of the implant, so the whole process feels smoother and more predictable.
When Implants Can Go In: Immediate, Early, or Delayed
Before we decide when to place an implant after an injury, we always look at how your jaw is healing. Everyone’s timeline is different, so we move at a pace that feels right for your long-term results.
Immediate
This is an uncommon option and works only when the fracture has healed perfectly, the bone feels strong, and the jaw segments are completely stable. For most individuals, we need a little more healing time before we can consider implants.
Early (6–12 weeks)
This timeline can work once the soft tissue has healed nicely and imaging shows that everything is stable. It keeps treatment moving while still giving your jaw a chance to recover.
Delayed (3–6+ months)
This is the most common route, especially in cases where bone grafting is required or when any hardware needs to be removed first. It gives the area time to regain its strength, so the implant has a better chance of succeeding.
We also work closely with your restorative dentist so that the final tooth design guides the entire surgical plan.
For many trauma cases, we recommend a staged approach to implants post-trauma to maximize long-term success.
Rebuilding the Foundation: Grafts, Plates, and Hardware
Once we understand what your jaw needs, we start rebuilding the foundation to ensure your implant has the strongest possible support. Sometimes this means ridge augmentation or a block graft to restore the width or height that was lost around the defect. In the upper back area, a sinus lift may be needed if trauma has reduced the available bone.
We also examine any plates or screws from your original treatment. Some can stay in place without affecting the plan, while others are better removed to create the right space for the implant. When necessary, soft tissue grafting can also help, especially if we need more keratinized tissue or want a natural, healthy emergence profile around the final tooth.
Surgical Techniques That Protect the Fracture Site
When planning implant surgery after a fracture, we are even more considerate of the protection of the area that has already healed. Guided surgery enables us to place the implant in the safest, most accurate position while avoiding old fracture lines and any hardware that may be in place. From there, we determine whether a short or narrow implant will work well or if it makes more sense to build up the area first with staged augmentation.
If more than one implant is required in that area, we sometimes use splinting techniques so that the implants support each other during healing. We also closely examine primary stability to decide whether the implant should be loaded with a temporary tooth right away or if waiting is better. With careful torque control and guided positioning, implants after jaw fracture can integrate predictably.
Risks, Red Flags, and How We Mitigate Them
Each time we place implants in a region that has experienced a fracture, we monitor for potential risks. The presence of a prior nonunion, decreased blood supply, residual infection, or nerves very close to the site can all influence how we plan your treatment.
We take a staged approach to grafts, use prophylactic antibiotics only when truly indicated, and employ a very gentle, atraumatic surgical technique to manage these risks. We also take you through a clear hygiene plan to keep healing predictable.
With time, we look for signs of success, including strong radiographic integration, stable and healthy probing depths, and a completely comfortable bite.
Recovery and What Results to Expect
Recovery after placement of an implant in an area that has been fractured before usually follows a steady and predictable rhythm. You can expect slight swelling and soreness at the start, then things will settle as your bone bonds with the implant. During this phase, your diet, hygiene, and follow-up visits matter even more than usual, so we guide you on exactly what to eat, how to keep the area clean, and when to check in with us.
At Ridge Oral Surgery in New Jersey, we also discuss whether a temporary tooth is immediately safe or if waiting will better protect the healing site. That balance between appearance and biology will make quite a difference. A thoughtful plan for implants post-trauma marries surgical precision with disciplined recovery protocol.
Why Choose Our Team for Trauma-Informed Implant Care
When you choose us for trauma-informed implant care, we start by mapping every detail with advanced CBCT planning and guided surgery so nothing is left to guesswork. We are also closely connected with your restorative dentist, so the final tooth you want shapes the entire plan.
Our team at Ridge Oral Surgery brings significant experience with grafts, hardware, and the challenges associated with prior fractures, helping make each successive step as smooth and predictable as possible.
Most importantly, we value your comfort and clarity about the process. From assessment to final restoration, we tailor implants after jaw fracture to your anatomy and goals.